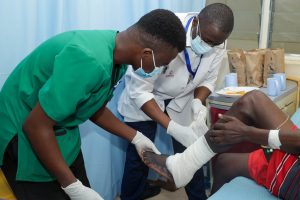
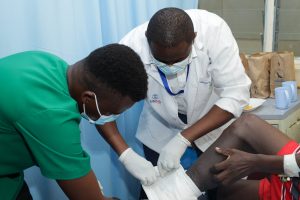
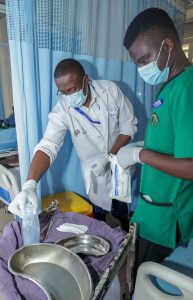
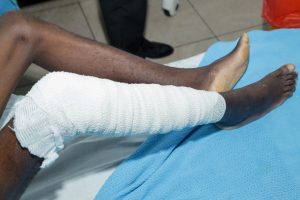
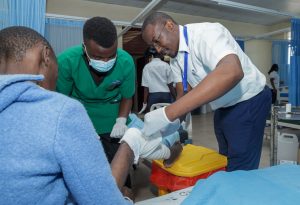
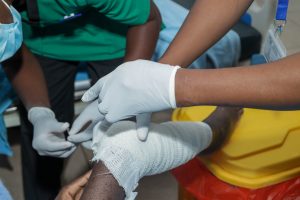
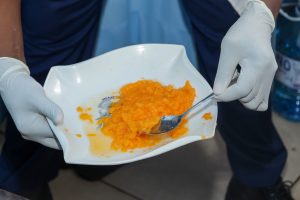
Story by Lorraine Opondo and Photos by Ondari Ogega
A new study by Dr. Silas O. Awuor has raised alarm over the growing threat of antimicrobial resistance (AMR) in wound care, warning that current treatment practices in Kenya may be doing more harm than good.
The research, conducted at Jaramogi Oginga Odinga Teaching and Referral Hospital, highlights that many wound infections are being treated using “empirical” methods — where doctors prescribe antibiotics without laboratory testing. According to the study, this approach is contributing to dangerously high levels of drug resistance.
The findings show that resistance to commonly used antibiotics such as ampicillin and cotrimoxazole now exceeds 90 percent in some cases. Even more concerning, the study reports increasing prevalence of methicillin-resistant Staphylococcus aureus (MRSA) and other hard-to-treat bacteria.
“Wound management continues to rely heavily on empirical antibiotic therapy, often without microbiological confirmation,” Dr. Awuor notes, pointing out that this practice accelerates the development of resistant pathogens.
“These infections are no longer responding to standard treatments,” the study notes, pointing to a widening gap between laboratory diagnostics and actual clinical decision-making.
The study highlights that chronic wounds, including diabetic ulcers and post-surgical infections, are increasingly hosting multiple bacteria at once, many of them resistant to available drugs. These infections are often complicated by biofilms, protective layers formed by bacteria that make them even more resistant to antibiotics.
The study identifies biofilms as a major barrier to healing. These protective bacterial communities are estimated to be present in a large majority of chronic wounds, such as diabetic foot ulcers.
Because biofilms increase bacterial tolerance to both antibiotics and the human immune system, standard drug treatments often fail unless they are paired with physical biofilm disruption, such as debridement.
Researchers warn that biofilms are a major reason why wounds fail to heal, despite ongoing treatment.
Kenyan healthcare workers have developed creative, low-cost solutions such as honey-based dressings, acetic acid applications for Pseudomonas infections, and improvised negative pressure wound therapy. While these innovations have improved access to care, the study says they are not enough to address the growing microbiological challenge.
A key issue is the limited use of diagnostic tools like culture and sensitivity testing, which help identify the exact bacteria causing infections and the most effective treatment.
The study calls for a nationwide shift toward what experts term “microbiological stewardship,” a system that prioritizes laboratory-guided treatment rather than guesswork.
This includes early diagnostic testing before prescribing antibiotics, closer collaboration between clinicians and microbiologists, and use of hospital-specific data to guide treatment decisions
Without these changes, researchers warn that antimicrobial resistance could continue to rise, leading to longer hospital stays, higher treatment costs, and increased patient deaths.
Antimicrobial resistance is already recognized as a global health crisis, but the study emphasizes that the impact is particularly severe in resource-limited settings like Kenya.
“The future of wound care depends on moving from guesswork to evidence-based healing,” the report concludes. Microbiological stewardship should be recognized as a central pillar in modern wound care,” the report also states, marking a necessary evolution in the fight against AMR in sub-Saharan Africa.